

Overweight and obesity in domestic cats: epidemiological risk factors and associated pathologies
J Feline Med Surg.
2024 Nov 19;26(11):1098612X241285519. doi:10.1177/1098612X241285519
This article is republished with permission from PubMed Central. The original article, "Overweight and obesity in domestic cats: epidemiological risk factors and associated pathologies,"
was published on 2024 Nov 19, and can be found on their website here: https://pubmed.ncbi.nlm.nih.gov/39560296/
Claudia Saavedra 1, Consuelo Pérez 1, Carlos Oyarzún 2, Ángelo Torres-Arévalo 1,✉
· Author information
· Article notes
· Copyright and License information
PMCID: PMC11577473 PMID: 39560296
Abstract
The domestic cat has evolved in various aspects in its journey from original domestication to the present day. Many domestic cats today lead a sedentary indoor lifestyle with low environmental stimulation. In addition, cats have changed their eating habits, transitioning from being carnivorous hunters to animals that eat commercial processed foods. Eating patterns have also changed since cats no longer need to hunt for food but instead have access to several portions throughout the day. All these variables, known as extrinsic epidemiological factors, added to animal-specific or intrinsic epidemiological factors (genetics, sex and breed, among others), predispose cats to the development of overweight and obesity (O&O). The prevalence of O&O has significantly increased in the global cat population, making them a growing clinical concern for companion animals. In turn, O&O contribute to the onset of other pathologies by either increasing susceptibility or creating conditions that allow existing or incipient pathologies to manifest or worsen. Some of these diseases correspond to changes in the musculoskeletal tissue, insulin resistance, type 2 diabetes, skin disorders, and kidney and urinary tract diseases, among others. Therefore, the aim of this review was to analyze the epidemiological variables and diseases associated with O&O in the domestic cat.
Keywords: Associated pathologies, epidemiological risk factors, overweight, obesity
Introduction
The domestication of cats has led to environmental, behavioral and nutritional changes, increasing the risk of developing diseases, such as overweight and obesity (O&O).1–3 O&O represent a major health problem for both humans and companion animals.4–6 In cats, O&O could be associated with a sedentary indoor lifestyle, ad libitum diet, excessive treats given by owners, male sex, neutering, middle age and owners underestimating their cat’s weight or body condition.7,8 In turn, the study of obesity has gained greater relevance as an important risk factor for the development of potentially fatal pathologies in cats (Figure 1).4,8
Figure 1.
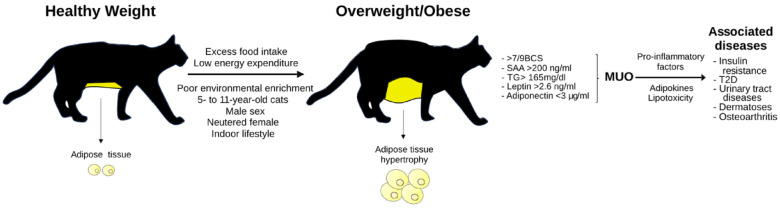
Risk factors, biological markers and associated pathologies for overweight and obesity (O&O) in domestic cats. Factors such as excessive food intake, low energy expenditure, poor environmental enrichment, age from 5 to 11 years, male sex, neutering and an indoor lifestyle predispose cats to the development of O&O. Certain overweight/obese cats (body condition score >7/9) that exhibit changes in biological markers (serum amyloid A [SAA], triglycerides [TGs], leptin and adiponectin) have been classified as metabolically unhealthy obese (MUO). MUO cats experience a significant weight gain with hypertrophy of adipose tissue, which favors the production and secretion of pro-inflammatory mediators and lipotoxicity due to adipokines, which predisposes to the development of associated diseases. T2D = type 2 diabetes
Overweight and obesity in the domestic cat
What is an overweight or obese cat?
Both O&O are becoming increasingly common in the cat population,8–11 with an estimated prevalence close to 40% in the USA and as high as 63% in other parts of the world, such as New Zealand.8,12–17
Overweight is defined as an excess of adipose tissue due to hypertrophy of adipocytes with the accumulation of triglycerides (TGs). This condition may be associated with metabolic deterioration and hormonal changes that affect quality of life and longevity.4,16,17 An overweight cat carries an excess weight of 10–19% over the ideal range.4,8,9 Obesity is a systemic, multiorgan, metabolic, chronic and progressive inflammatory fat disease, influenced by the interplay between genomic and environmental factors. This condition poses great risk of morbidity and mortality. 18 In cats, obesity is considered an excess weight of greater than 20–30% of the ideal range.4,8,9
In veterinary medicine, body condition score (BCS) is the most common method used in research and practice to semi-quantitatively measure the superficial body condition of cats.19–22 A half-number from 1 to 5 or a whole number from 1 to 9 is assigned based on the physical characteristics of the patient, evaluating whether it is possible to visualize and palpate the ribs, waist, abdomen, spine and pelvis according to the amount of fat present. 19 Some authors have determined that each BCS point over the healthy weight represents an increase of 7–10% in body weight.11,22 On the BCS 9-point scale, a score of 1 indicates emaciation, while scores of 2–4 are given when the patient is underweight. A score of 5 represents an ideal or healthy body condition. Scores of 6–7 indicate that the patient is overweight, and scores of 8–9 suggest obesity. 19 However, the current World Small Animal Veterinary Association (WSAVA) BCS chart includes a footnote caveat that a BCS of 6/9 may be appropriate for many cats, especially older ones. 21 In fact, a study carried out by Teng et al 19 identified increased survival time in middle-aged cats with a BCS of 6/9, suggesting that this score is optimal for a healthy condition in cats.
Another indicator of O&O is body mass index (BMI), a method for predicting body fat content in cats through body measurements (zoometric) with the cat in a standing position and its four limbs perpendicular to the floor. 23 In the rib cage, at the ninth cranial vertebra, the circumference should be measured in centimeters (cm), and, in addition, the leg index measurement should be performed by quantifying the distance, in cm, between the patella and the calcaneal tuberosity in the left hind limb. Finally, the percentage of body fat content is obtained from the equation in Figure 2. 23
Figure 2.
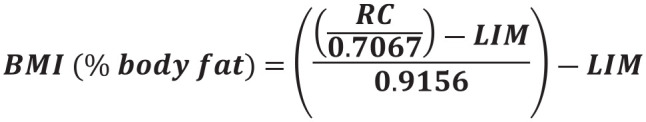
Equation to calculate body mass index (BMI) in cats. This formula estimates the body fat percentage in cats through the rib cage (RC) measurement and the leg index measurement (LIM) in centimeters
A cat with a BMI of 10–29% is considered to have a healthy weight, while a BMI of 30% or higher indicates overweight or obesity. 23
The BCS of a cat does not always accurately reflect body fat distribution, prompting further investigations. One such investigation estimated fat distribution in the body using CT. 24 Identifying fat distribution through CT allows for the determination of the amount of abdominal fat, which has been associated with lipotoxicity and metabolic complications in obese cats. 24 Okada et al 24 evaluated how the visceral fat area (VFA):subcutaneous fat area (SFA) ratio measured using CT correlated with metabolic, hormonal and enzymatic profiles in 10 client-owned cats with varying BCSs. High VFA:SFA ratios were observed in obese cats (BSC >7/9) with modifications in serum adiponectin, TGs and serum amyloid A (SAA) concentrations. These results suggest that a pathologically or metabolically unhealthy overweight/obese (MUO) cat can be diagnosed in the clinic if it has two or more of the following signs: low serum adiponectin concentration (<3 μg/ml); hyperlipidemia (TGs >165 mg/dl); and high levels of SAA (>200 ng/ml) (Figure 1). Thus, the authors assert a new classification in which O&O cats (BCS >7/9) with and without inflammatory reactions should be classified as obesity disease (MUO) and simple obesity (metabolically healthy obesity [MHO]), respectively. 24 In this way, the search for new O&O markers has led recent research to focus on identifying epidemiologic risk factors that allow a better understanding of the development of O&O in domestic cats.
Epidemiologic risk factors in overweight and obese domestic cats
There are several risk factors associated with O&O in domestic cats; these can be classified into intrinsic and extrinsic (Tables 1 and 2).30,32 Intrinsic factors include breed, sex, age, neutering and genetic changes.18,32 Extrinsic risk factors are related to the environment and management conducted by cat owners, with the type of diet, as well as the amount and frequency of feeding, being some of the most relevant.15,16,32 Another key extrinsic factor in feline obesity is a sedentary lifestyle, as many obese cats are found in small spaces without stimuli or environmental enrichment, thus reducing the animal’s energy expenditure. 4 These factors generate a heightened risk of developing obesity, which, in turn leads to various health consequences for domestic cats.
Table 1.
Epidemiologic risk factors associated with overweight and obesity in domestic cats
| Intrinsic factors | Extrinsic factors |
| Sex (male) | Feeding (dry food fed ad libitum) |
| Breed (DSH, mixed breed, British Shorthair, Maine Coon and Norwegian Forest Cat) | Cat–owner relationship (more affection and humanization, underestimation of BCS) |
| Age (middle age) | Low physical activity (sedentarism) |
| Sterilization (neutered) | Company of other animals (competition/stress) |
| Genetic disorders | Indoor lifestyle |
Open in a new tab
BCS = body condition score; DSH = domestic shorthair
Table 2.
Research articles about epidemiological risk factors associated with oveweight and obesity (O&O) in domestic cats
| Title | Most relevant findings | Reference |
| Prevalence and risk factors of obesity in an urban population of healthy cats | This study found that in a population of healthy cats, 19% were overweight and 7.8% were obese. It was concluded that owners understand a visual BCS scale better than a verbal scale. Characteristics such as male sex, neutering and underestimation of BCS by owners are considered risk factors for O&O in cats. | Colliard et al, 2009 25 |
| Trained vs untrained evaluator assessment of body condition score as a predictor of percent body fat in adult cats | This study revealed that body fat percentages increased ~7% for each half-point of BCS over 3 points, using the 5-point scale. The veterinarian had the strongest correlation coefficient between BCS and fat percentage than the veterinary technician, trained scorer and untrained scorer. | Shoveller et al, 2014 22 |
| Post-castration variations in weight gain in a cohort of young adult male cats | In this study, weight gain after castration was identified as a risk factor. The individual weight gain at 6 months after castration was in the range of 3–53%. | Wei et al, 2014 26 |
| Obesity in show cats | In this study, the largest population of cats were classified with BCS 6/9 (45.5%); most of these animals evaluated belonged to the group of neutered cats. Breed standards could influence BCS estimation. Neutering predisposes to obesity and requires early nutritional intervention to prevent it. | Corbee, 2014 7 |
| Risk factors identified for owner-reported feline obesity at around one year of age: dry diet and indoor lifestyle | This study described that 7% of the 966 cats evaluated were O&O between 12.5 and 13 months of age, with their condition mainly associated with a dry diet and restricted or no access to the outdoor environment. | Rowe et al, 2015 4 |
| Metabolic profiling reveals effects of age, sexual development and neutering in plasma of young male cats | This study described how, after neutering, changes in the cat’s energy expenditure and consumption occur; also how metabolism is acutely decreased after castration. Feline metabolism is the most significantly altered pathway, increasing during sexual development and decreasing acutely after castration. | Allaway et al, 2016 27 |
| Overweight adult cats have significantly lower voluntary physical activity than adult lean cats | This research found that overweight cats (>3/5) only achieve 60% of the voluntary physical activity performed by healthy weight and underweight cats (BSC ⩽3/5). Overweight cats have lower anxiety around social contact with humans than cats with a BSC ⩽3/5. | de Godoy and Shoveller, 2017 28 |
| Owner and cat-related risk factors for feline overweight or obesity | Through an international survey, this study found that owners with low conscientiousness are at a greater risk of having O&O cats. Therefore, the owner has an important role in the prevention of obesity. | Wall et al, 2019 15 |
| Brazilian owners perception of the body condition score of dogs and cats | In this study, it was observed that is difficult for owners to assess BCS, particularly for owners from rural areas. | Teixeira et al, 2020 29 |
| Positive attitudes towards feline obesity are strongly associated with ownership of obese cats | Owners with an approving attitude towards O&O or owners who consider ‘being chubby or fat with a good quality of life’ have a greater risk of their cat suffering from O&O, unlike those with a disapproving attitude. Certain characteristics of cats have been described, such as being middle-aged, mixed breed, eating dry food, not quantifying food and living indoors, which are associated with a higher incidence of O&O. | Teng et al, 2020 30 |
| Beloved whiskers: management type, care practices and connections to welfare in domestic cats | Although an indoor lifestyle is related to a closer relationship between the owner and the cat, it is also associated with higher rates of obesity and owner-reported behavioral problems compared with cats that lead an outdoor lifestyle. | Machado et al, 2020 31 |
Open in a new tab
BCS = body condition score
Intrinsic epidemiological factors
Breed
Certain authors mention that purebred cats, such as Abyssian, Cornish Rex and Sphynx cats, among others, have the lowest risk of obesity compared with domestic longhair, domestic shorthair and crossbred cats.15,33 In fact, studies have shown that crossbred cats tend to have a higher BMI than purebred cats.14,34 Among the breeds investigated, only the British Shorthair appears to be more susceptible to being overweight. 34 Corbee 7 indicates that Maine Coons and Norwegian Forest Cats are also predisposed to being O&O. However, comparisons between purebred and crossbred cats may be biased, since the number of purebred cats in the study groups is lower than that of the crossbreeds. 34 In addition to breed, fur length is also considered a variable that has been associated with under- or overestimation of BCS by owners. 34
Age
The average presentation of O&O in cats is 8.3 years; however, most studies describe obesity in populations aged 5–11 years, with few describing obesity in young cats.14,35 However, for young and strictly indoor cats, the risk of developing O&O appears as early as 12–13 months of age. 4
Recent studies have confirmed that the increase in body weight is associated with increasing age and is correlated with an increase in serum glucose, TGs and SAA. 36
Sex and neutering
The relationship between O&O and sex is mixed. In intact cats, male cats consume more metabolizable energy (ME) and gain weight more easily than female cats.14,37 Then, in both sexes, neutering is an important factor predisposing to the development of O&O, 15 especially when daily calorie intake is not being controlled.14,37 However, after neutering, the risk of O&O is higher in females than in males.16,37 The effect of sex is further complicated by the fact that females tend to live longer, while males tend to have a higher body weight. 38
The extraction of the gonads reduces the secretion of estrogens, which increases appetite, decreases energy requirements and consequently increases voluntary food consumption, thereby raising the risk of weight gain.8,26,27 In a study conducted by Wei et al, 26 freely fed cats showed body weight gains of up to 17% and 43% 1 and 3 months after neutering, respectively. Other studies have also shown that free-demand feeding has a strong effect on weight gain and body fat percentage in neutered cats, regardless of the age of neutering. 27
Extrinsic epidemiological factors
Diet
Food moisture content
Research indicates that cats eating predominantly dry food (⩾75% of its feed is dry food) are up to 2.4 times more likely to be overweight than those on a predominantly wet diet (⩾75% of its feed is wet food). 14 Further research has shown that cats fed from an early age with food comprising more than 50% dry food have up to a 79% risk of being overweight or obese. 4 In fact, cats fed wet food ad libitum have better body condition than those that are fed only dry food and/or wet food at fixed times. 4 In addition, it has been determined that regardless of the feeding style (fixed schedule or ad libitum), dry feeding alone predisposes to O&O. 4 Thus, weight gain and food intake could be related to moisture content in food. 39
Components: macronutrients
In the wild, cats are primarily carnivores, which implies a diet that is very low in carbohydrates (<3% of the ME), moderate in fat content (~46% of the ME) and especially high in protein (~52% of the ME; up to 62.19% of crude protein content on a dry basis).40–42 However, available commercial food formulas vary widely, with carbohydrate content sometimes contributing up to 45% of ME for technical and economic reasons. 41 Notably, some authors have stated that cats adjust their food intake to achieve a diet with a daily energy intake composition close to 52% of protein (420 kJ/d), 36% of fat (280 kJ/d) and 12% of carbohydrates (100 kJ/d) when given the choice.42,43 That suggests that domestic cats have mechanisms for sensitive metabolic regulation that help them reach a macronutrient intake similar to that of wild cats. 42
Currently, commercially available foods do not match the same carbohydrate content as a cat’s natural prey diet. Studies suggest that this excess in carbohydrates leads to an overproduction of insulin, which increases body fat in cats. This further supports the idea that the difference between current food formulas and a natural diet may be the primary cause of feline obesity. 40 It is important to note that some studies associating the components (carbohydrate, protein and lipids) and type (dry and/or wet) of cat food and frequency of feeding are mostly based on surveys conducted with owners and do not consider or control the calorie intake in the cat’s diet.
To better understand the impact of eating habits in cats, we studied the effects of a high-carbohydrate/low-protein (HC/LP; nutrient composition [g/100 g]: 38.1 and 27.5 of carbohydrate and protein, respectively) and high-protein/low-carbohydrate (HP/LC; nutrient composition [g/100 g]: 24.7 and 45.2 of carbohydrate and protein, respectively) isoenergetic diets on glucose and fat metabolism. Hoenig et al 44 evaluated 12 healthy weight and 16 obese cats before and after weight loss for this purpose and found that the HP/LC diet maintains normal insulin sensitivity and facilitates the reduction of body fat during weight loss. Nevertheless, the authors also reported that dietary protein and carbohydrate content were not related to severe insulin resistance in cats, although dietary content based on ME was not evaluated in this study. In addition, research by Verbrugghe et al 45 assessed the impact of three homemade diets on glucose tolerance and insulin response in cats. The diets were designed to be isoenergetic and each with a distinct reduction in one of the energy-contributing macronutrients (protein, fat and carbohydrates measured as nitrogen-free extract [NFE]), and were thus classified into LP (28%, 43% and 29% of protein, fat and NFE as ME, respectively), low-fat (LF; 47%, 27% and 25% of protein, fat and NFE as ME, respectively) and LC (45%, 48% and 7% of protein, fat and NFE as ME, respectively) diets. The authors described no variation in both plasma glucose concentrations and the area under the glucose curve between conditions; however, cats fed an LP diet showed a diminished area under the insulin curve, while a delayed second insulin peak was observed in cats fed the LC diet. These findings suggest that reducing carbohydrate content in commercially available foods could trigger an insulin-resistant state, which the authors attribute to the strictly carnivorous nature of cats. The study even implies that proteins might have a negative impact on insulin sensitivity, pointing to the highly gluconeogenic aspects of amino acids in strict carnivores. 45 Considering these results, carbohydrate consumption does not appear to be a main factor in the development of obesity in cats; hence, additional research has focused on proteins and fats as the variable to be evaluated in the diet. Investigations have shown that neutered cats with free access to an LC/high-fat (HF) diet (340 g/kg of NFE and 206 g/kg of fat; 18.4 MJ of ME/kg) experience weight gain and increased body fat mass compared with those on an HC/low-fat (LF) diet (403 g/kg of NFE and 109 g/kg of fat; 14.4 MJ of ME/kg). 46
Recent studies conducted by Mo et al 47 evaluated the impact of varying fat levels (8% or 16% on a fed basis) and starch sources (pea starch or corn starch) on body weight, glycolipid metabolism, hematology and fecal microbiota in clinically healthy cats. After 28 days, cats consuming HF diets exhibited an average weight gain of 50 g more than those on LF diets. Furthermore, hematological analysis revealed increased inflammation in cats fed HF diets. Glucose and insulin levels were lower in cats on LF diets compared with those on HF diets. In addition, cats on HF diets showed higher serum concentrations of total cholesterol, TGs and high-density lipoprotein (HDL) cholesterol than those on LF diets. 47
Taken together, the data suggest that high dietary fat, rather than carbohydrates, induces increased body weight alongside elevated insulin levels. Therefore, Godfrey et al 39 recommend growth diets with lower energy density to prevent obesity in cats.
In addition, Coradini et al 48 compared an HP/LC diet (47% and 23% of ME for protein and carbohydrates, respectively) against an HC/LP diet (51% and 21% of ME for carbohydrate and protein, respectively) with similar energy density (1552 and 1550 kJ/100g for HP/LC and HC/LP, respectively), and found that cats fed the HP/LC diet ad libitum had both increased fat deposition and enhanced weight gain. It is worth mentioning that these outcomes might be due to higher fat content in the HP/LC diet or from cats self-regulating their carbohydrate intake, thereby moderating their energy consumption when fed HC/LP diets.40,41
Overfeeding and thereby consumption of excess calories from any macronutrient is a much more important risk factor for obesity and should be the focus of obesity prevention. 39 There is a need to improve owner education with a focus on feeding a measured amount of food appropriate for each cat’s individual energy requirements, considering factors such as spay/castration status, aging and inactive lifestyle, which reduce energy requirements. 39 Attention should also be paid to feeding strategies that provide environmental enrichment and increase physical activity.39,40
Lifestyle and physical activity
In domestic cats, an indoor lifestyle increases the chances of obesity and higher BCS compared with those with a mixed or outdoor lifestyle.15,31 In this way, cats with little to no access to the outdoor environment from a young age are twice as likely to become O&O as a result of decreased physical activity, leading to boredom and consequently to greater food consumption. 6 In addition, indoor cats that live with other cats are prone to higher and chronic stress levels, which leads to higher caloric intake. 15 Therefore, outdoor cats that have a more stimulating environment are less likely to get bored and overeat. 15
In 2014, Shoveller et al 22 described a decrease in physical activity during the day in neutered cats, leading to an increase in body weight and lower energy expenditure. Another study reported that overweight cats perform less voluntary physical activity than healthy weight cats and that this is also influenced by the presence or interaction with humans. 28 In addition, healthy weight cats are primarily active at night, before eating and are more anxious in social interactions with their owners. 28
Low levels of physical activity also correlate with an increased likelihood of developing certain metabolic diseases associated with O&O, including type 2 diabetes (T2D). 28
Owner’s perception of the cat’s status/cat–owner relationship
It has been described that owners who show more affection and humanizing traits and who associate O&O with tenderness or cuteness (rounded body structure and body fat) and consider it to be a positive trait are more likely to have an overweight or obese cat.30,49 This would indicate that the behavior of the owners and their education about O&O in cats are crucial factors in controlling the development of these metabolic pathologies, as the caretaker is responsible for the great majority of the cat’s food intake. In fact, Wall et al 15 recently demonstrated that low owner conscientiousness was associated with an increased risk of feline O&O, whereas a preference for delayed reward and indulgent and inconsistent feeding practices were associated with a decreased risk. In accordance with human studies, the indulgent and inconsistent feeding practices could be expected to pose a risk for the development of O&O;50,51 however, in the study by Wall et al, these habits appeared protective in cats. 15 To explain this, the authors proposed that these owners would also be more concerned about the health and body condition of their cat and the amount of food offered, likely owing to their use of probably expensive diets and treats. Moreover, these owners usually provide a wide variety of foods that could decrease overfeeding associated with boredom and begging. 15
In addition, various studies in Europe and South America have reported that cats with higher BCS had owners who undervalue their body condition.12,25,29,30,52 The underestimation of the BCS may be due to a lack of understanding of the verbal scale, as other studies have reported lower BCS on the verbal scale compared with the visual scale. 25 However, owners who have had nutritional consultations or possess prior knowledge of the subject tend to report greater compliance with the BCS as estimated by the veterinarian. 29
Studies show that cats that frequently ask for food are five times more likely to be overweight or obese than cats that do not. This group includes cats that do not beg for food but are misinterpreted and overfed by their caretakers, leading to a cycle in which the cat adopts a certain behavior to be rewarded with food by the owner. 30 Thus, begging for food is associated with an increase in the cat’s energy intake without an increase in energy expenditure. 30
Finally, it is important to point out that most owners view O&O as negative or disapproving conditions; however, they often overlook the associated consequences and negative effects on their cats’ health. 30 Therefore, preventive medicine should focus on educating caretakers about the estimation of BCS, for the early detection of O&O, to prevent the development of associated pathologies.
Consequences of overweight and obesity in domestic cats: associated pathologies
As in human medicine, Okada et al 24 proposed that obesity in domestic cats should be classified into two major groups: (1) MHO, which corresponds to obese cats without significant health issues; and (2) MUO, in which patients experience associated diseases.
The term MHO began to be proposed in the 1950s, based on findings from a subgroup of obese human patients who showed a lower risk of developing pathologies such as T2D and atherosclerosis.53,54 Typically, a human MHO patient is defined as one who does not present with metabolic (eg, T2D, dyslipidemia, fatty liver disease) or cardiovascular (eg, hypertension, myocardial infarction, stroke) complications; however, other researchers have used other criteria (plasma TGs, total cholesterol, HDL cholesterol, low-density lipoprotein [LDL] cholesterol and C-reactive protein levels and glucose tolerance test, among others), which has complicated the interpretation and unification of results.54–56 It is important to note that human MHO patients should not be considered or classified as a benign sub-phenotype of obesity, since recent data from large epidemiological studies and meta-analyses have shown that MHO individuals have a higher risk of cardiometabolic complications compared with metabolically healthy weight individuals. 54
In feline medicine, the only approximation to the MHO concept was a study published in 2019 by Okada et al, 24 which identified a subgroup of obese cats (BCS >7/9) with normal levels of TGs and liver enzyme activities, and high and low plasma adiponectin and SAA concentration, respectively. 24 More studies should be carried out in MHO cats in order to characterize and identify possible health risks in these animals.
Various studies that have been carried out on O&O domestic cats suggest that ophthalmic disorders, non-allergic skin diseases, digestive system disorders, lameness, hepatic lipidosis, heart diseases, insulin resistance, T2D and urinary system disorders are the most frequent pathologies associated with MUO patients.8,10,14,24,34,57,58 However, it is important to note that a common etiology or underlying factor could be related to all of these pathologies, and they do not necessarily have a causal relationship with MUO in cats.
As a result of O&O, multiple metabolic and/or mechanical disorders can develop in domestic cats. 16 Metabolic disorders may include an increase in the production of metabolites of adipose tissue and an increase in the number of inflammatory cells.16,59 Mechanical disorders, on the other hand, are due to the excessive accumulation of fat, which produces a greater load on the joints and overexerts the heart, contributing to the development of degenerative conditions in both the heart and joints of O&O cats. 16
Another possible alteration that comes with O&O is dyslipidemia, a condition characterized by high blood concentrations of cholesterol and TGs. 16 Both molecules are transported in the blood by HDLs, LDLs and very low-density lipoproteins (VLDLs). 60 In the case of obesity, levels of VLDL and fatty acids are increased in the blood of animals.16,61 When fatty acid concentrations rise, protein kinases involved in insulin receptor function are activated, which can lead to insulin resistance and T2D.16,62 In addition, some studies in cats mention that the accumulation of visceral fat is a risk factor for metabolic syndromes, high blood pressure and some types of cancer. 24
Some of the main diseases associated with O&O in domestic cats are described below.
Urinary tract disorders and kidney disease
Some of the most common urinary tract diseases seen in O&O cats are urolithiasis, lower urinary tract disease (LUTD) and cystitis. 14
Obesity has been associated with increased excretion of minerals in the urine, 63 increased food intake and increased susceptibility to urolithiasis. 64 Neutering and an indoor lifestyle, although not exclusive to obese patients, have also been linked to urinary tract disorders such as urolithiasis.63,65
It has been suggested that struvite uroliths would be more frequent in obese cats because they likely consume a greater amount of chalcogen minerals and drink less water. 64 Moreover, indoor and neutered cats tend to consume less water, engage in less physical activity and produce less urine. 65 This leads to urine remaining in the bladder for longer periods, predisposing animals to the formation of uroliths and urinary tract infections. 64 Indeed, neutered cats have an 8.3 times higher risk of presenting with uroliths than non-neutered cats. 63
In human medicine, obesity, prediabetes and T2D predispose to chronic kidney disease (CKD);66,67 however, this association has not been fully investigated in cats. A study conducted on 54 clinically healthy cats evaluating markers for CKD, such as symmetric dimethylarginine (SDMA), serum creatinine, urine specific gravity (USG), urine protein:creatinine (UPC) ratio, urinary free active transforming growth factor-β1:creatinine ratio and urinary retinol binding protein:creatinine ratio, found no association between BCS and these markers. 66
Skin disease
Estimates suggest that an overweight or obese cat is up to 2.3 times more likely to develop unspecified dermatopathy and non-allergic skin disease than a healthy weight cat.68,69 Obese cats can develop dermatologic pathologies due to secondary chronic inflammatory and metabolic alterations. 34 In addition, several authors mention that obese cats have difficulty grooming hard-to-reach areas and, therefore, are at a higher risk for developing dermatosis.34,68
Obesity can increase water loss, leading to a disruption of the epithelial barrier function and causing chronic generalized inflammation, which could trigger or worsen atopic dermatitis. 70
In addition, some of the treatments for dermatologic conditions involve the use of corticosteroids, which may increase appetite. This suggests that O&O could be a consequence of dermatosis treatment and/or vice versa. 34
Osteoarthritis and degenerative joint disease
Joint deterioration is caused by synovial inflammation and chondrocyte damage through the secretion of inflammatory mediators, such as TNF-α and interleukins (IL-1 and IL-6), as well as hormones like leptin and adiponectin. 71 Many of these molecules correspond to adipokines, so the increase in adipose tissue could contribute to the development of systemic and local inflammatory processes such as osteoarthritis. There is substantial evidence in humans and dogs suggesting a correlation between obesity and osteoarthritis and degenerative joint disease; however, this relationship has not yet been established in cats,57,68,72–75 although it has been proposed that excessive weight gain significantly affects the joints by generating mechanical overload.71,76
Nonetheless, Mianiaki et al 77 recently identified O&O as risk factors for owner-reported mobility changes in pet cats at 6 years of age by researching prospective data from a longitudinal cohort study from the UK.
Heart and respiratory diseases
Hypertrophic cardiomyopathy (HCM) is the most prevalent heart disease in domestic cats, accounting for 60% of all heart diseases that affect cats. 78
It has been described that obesity does not have a strong correlation with the presentation of heart disease such as HCM in cats, since previous studies found body weight and BCS to be irrelevant.78,79 Indeed, unlike humans, obese cats with high plasma VLDL levels do not develop hypertension and atherosclerosis.3,80 However, it remains a possibility that these cats were obese before presenting with heart disease. 78 Although obesity is not considered a risk factor, a study of cats with heart failure by Finn et al 81 identified that heavy body weight was associated with a lower survival rate than intermediate body weight.
Studies on the correlation between O&O and pulmonary function in cats have yielded contradictory results. Investigations that evaluated cats with bronchial disease divided into healthy weight and O&O groups through plethysmography showed no differences in lung function parameters according to body condition. 78 These parameters included tidal volume, expiratory and inspiratory times, maximum pressures, partial pressures of CO2 and O2, and respiratory rate. 78 On the contrary, using barometric whole-body plethysmography, García-Guasch et al 82 demonstrated that obesity impairs pulmonary function in cats, although a significant increase in bronchoconstriction indexes was not observed. In another recent investigation, Caro-Vadillo et al 83 evaluated the impact of obesity on the lung function of 53 cats with bronchoconstriction. In that study, overweight cats presented lower tidal volume, minute volume, and both inspiratory and expiratory flows compared with healthy weight cats. These results suggest that overweight cats have diminished lung function parameters indicative of a restrictive pattern compared with healthy weight cats. However, overweight cats did not show a higher bronchoconstriction level compared with healthy weight cats. Therefore, the lung function of an overweight cat is associated with a restrictive pattern without correlation with bronchoconstriction. 83
Moreover, inflammatory diseases of the lower respiratory tract and asthma are common in domestic cats; however, unlike in humans, O&O are not recognized as risk factors for these respiratory pathologies.78,83,84 Despite this, it has been determined that obesity leads to a decrease in the secretion of adiponectin and an increase in leptin in the blood, which could be related to the increase in the neutrophilic bronchial inflammation. 83
Insulin resistance and diabetes mellitus
As previously mentioned, a dysregulation in the plasma concentration of adipokines has been observed in obese cats,24,44 which could impact the development of insulin resistance and diabetes. 85 Insulin resistance corresponds to a decreased sensitivity of the body to respond to the effects of insulin, in which the concentration–response relationship of insulin is altered, requiring high blood levels of this hormone to exert its effects in target organs. 8 High blood insulin levels can be identified in feline patients that experience an increase of 7–10% of their ideal weight.22,86 In a study conducted by Hoenig et al, 44 it was possible to determine, using a hyperinsulinemic-euglycemic clamp, that for each kilogram of extra weight, insulin sensitivity decreased by 30%. Other research compared indices of glucose disposal and insulin sensitivity before and after 10 months of controlled weight gain in 16 cats. 87 In that study, feline obesity was associated with a 52% decrease in tissue sensitivity to insulin and a reduction in glucose efficiency. Surprisingly, healthy weight cats with low insulin sensitivity and glucose efficiency had a greater risk of developing glucose intolerance after becoming obese. Male cats gained more weight than female cats, which, together with low insulin sensitivity and higher insulin concentrations, puts them at greater risk of diabetes. 87 Diabetes in cats is a disease primarily associated with obesity, with a prevalence of 0.4% in the UK, 10 with T2D or insulin resistance being the most frequent types, accounting for 80% of the total population of diabetic cats. 10 Obese cats are 2–4 times more likely to develop diabetes. 8
In addition, obesity decreases insulin binding sites on its receptors and reduces the body’s ability to respond to it, leading to insulin resistance due to defects in glucose metabolism. 87
Hyperinsulinemia associated with T2D predisposes cats to cell proliferation and neoplastic growth; 10 however, although the association between obesity and cancer is well documented in humans, there are few data describing it in veterinary medicine.
Conclusions
An increase in the prevalence of O&O in domestic cats has been observed, which has been associated with various epidemiological risk factors classified as intrinsic (specific to the animal) and extrinsic (including diet, lifestyle and the owner–cat relationship). O&O predisposes mostly to insulin resistance, T2D, urinary tract disorders and skin, articular and kidney diseases.
Therefore, early dietary and feeding management strategies, such as avoiding HF ad libitum diets, must be implemented for obesity prevention. The education of owners regarding the body condition and the consequences of O&O in domestic cats seems to be crucial to prevent or treat the complications associated with these conditions.
Currently, in clinical practice, the diagnosis of overweight or obese cats can be established based on BCS (⩾7/9), BMI (⩾30%) and TG levels (>165 mg/dl). However, in recent years, different strategies have been used to characterize an overweight or obese cat, leading to the classification of MHO and MUO cats. A cat will be diagnosed as MUO if it presents with a BCS >7/9, low serum adiponectin concentration, hyperlipidemia and high levels of SAA. The literature indicates that MUO cats evaluated using CT present a greater accumulation of adipose tissue at the abdominal level, which has been associated with lipotoxicity events and the development of various pathologies. Therefore, future studies should not only evaluate the body condition of the overweight or obese patients, but also examine the distribution of adipose tissue to identify new techniques for assessing obesity in clinical practice.
Finally, we consider that future research should be focused on the characterization of MHO and MUO cats and the study of their physiopathology and associated diseases.
Footnotes
Accepted: 31 August 2024
The authors declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Funding: This article was funded by a grant (11230660) from FONDECYT of Chile to one of the authors (ÁTA).
Ethical approval: This work did not involve the use of animals and therefore ethical approval was not specifically required for publication in JFMS.
Informed consent: This work did not involve the use of animals (including cadavers) and therefore informed consent was not required. No animals or people are identifiable within this publication, and therefore additional informed consent for publication was not required.
ORCID iD: Ángelo Torres-Arévalo https://orcid.org/0009-0009-8956-6724
References
· 1. Miyazaki T, Sasaki SI, Toyoda A, et al. Influences of taurine deficiency on bile acids of the bile in the cat model. Adv Exp Med Biol 2019; 1155: 35–44. [DOI] [PubMed] [Google Scholar]
· 2. Forman MA, Steiner JM, Armstrong PJ, et al. ACVIM consensus statement on pancreatitis in cats. J Vet Intern Med 2021; 35: 703–723. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 3. Hoenig M. The cat as a model for human obesity and diabetes. J Diabetes Sci Technol 2012; 6: 525–533. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 4. Rowe E, Browne W, Casey R, et al. Risk factors identified for owner-reported feline obesity at around one year of age: dry diet and indoor lifestyle. Prev Vet Med 2015; 121: 273–281. [DOI] [PubMed] [Google Scholar]
· 5. Wallis N, Raffan E. The genetic basis of obesity and related metabolic diseases in humans and companion animals. Genes (Basel) 2020; 11. DOI: 10.3390/genes11111378. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 6. Koenen M, Hill MA, Cohen P, et al. Obesity, adipose tissue and vascular dysfunction. Circ Res 2021; 128: 951–968. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 7. Corbee RJ. Obesity in show cats. J Anim Physiol Anim Nutr (Berl) 2014; 98: 1075–1080. [DOI] [PubMed] [Google Scholar]
· 8. Clark M, Hoenig M. Feline comorbidities: pathophysiology and management of the obese diabetic cat. J Feline Med Surg 2021; 23: 639–648. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 9. German AJ. The growing problem of obesity in dogs and cats. J Nutr 2006; 136: 1940S–1946S. [DOI] [PubMed] [Google Scholar]
· 10. Chandler M, Cunningham S, Lund EM, et al. Obesity and associated comorbidities in people and companion animals: a one health perspective. J Comp Pathol 2017; 156: 296–309. [DOI] [PubMed] [Google Scholar]
· 11. Shepherd M. Canine and feline obesity management. Vet Clin North Am Small Anim Pract 2021; 51: 653–667. [DOI] [PubMed] [Google Scholar]
· 12. Cave NJ, Allan FJ, Schokkenbroek SL, et al. A cross-sectional study to compare changes in the prevalence and risk factors for feline obesity between 1993 and 2007 in New Zealand. Prev Vet Med 2012; 107: 121–133. [DOI] [PubMed] [Google Scholar]
· 13. Vandendriessche VL, Picavet P, Hesta M. First detailed nutritional survey in a referral companion animal population. J Anim Physiol Anim Nutr (Berl) 2017; 101: 4–14. [DOI] [PubMed] [Google Scholar]
· 14. Öhlund M, Palmgren M, Holst BS. Overweight in adult cats: a cross-sectional study. Acta Vet Scand 2018; 60: 5. DOI:10.1186/s13028-018-0359-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 15. Wall M, Cave NJ, Vallee E. Owner and cat-related risk factors for feline overweight or obesity. Front Vet Sci 2019; 6. DOI: 10.3389/fvets.2019.00266. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 16. Witzel AL. Comorbidities associated with obesity. In: Ettinger SJ, Feldman EC, Côté E. (eds). Textbook of veterinary internal medicine: diseases of the dog and the cat. 8th ed. St Louis, MO: Elsevier, 2017, pp 2171–2174. [Google Scholar]
· 17. Zhao J, Zhou A, Qi W. The potential to fight obesity with adipogenesis modulating compounds. Int J Mol Sci 2022; 23. DOI: 10.3390/ijms23042299. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 18. Lin X, Li H. Obesity: epidemiology, pathophysiology, and therapeutics. Front Endocrinol (Lausanne) 2021; 12. DOI: 10.3389/fendo.2021.706978. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 19. Teng KT, McGreevy PD, Toribio JL, et al. Strong associations of nine-point body condition scoring with survival and lifespan in cats. J Feline Med Surg 2018; 20: 1110–1118. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 20. Martins TO, Ramos RC, Possidonio G, et al. Feline obesity causes hematological and biochemical changes and oxidative stress – a pilot study. Vet Res Commun 2023; 47: 167–177. [DOI] [PubMed] [Google Scholar]
· 21. World Small Animal Veterinary Association. Body condition score. https://wsava.org/wp-content/uploads/2020/08/Body-Condition-Score-cat-updated-August-2020.pdf (2020, accessed 11 April 2024). [Google Scholar]
· 22. Shoveller AK, DiGennaro J, Lanman C, et al. Trained vs untrained evaluator assessment of body condition score as a predictor of percent body fat in adult cats. J Feline Med Surg 2014; 16: 957–965. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 23. Butterwick R. How fat is that cat? J Feline Med Surg 2000; 2: 91–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 24. Okada Y, Ueno H, Mizorogi T, et al. Diagnostic criteria for obesity disease in cats. Front Vet Sci 2019; 6. DOI: 10.3389/fvets.2019.00284. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 25. Colliard L, Paragon BM, Lemuet B, et al. Prevalence and risk factors of obesity in an urban population of healthy cats. J Feline Med Surg 2009; 11: 135–140. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 26. Wei A, Fascetti AJ, Kim K, et al. Post-castration variations in weight gain in a cohort of young adult male cats. J Nutr Sci 2014; 3. DOI: 10.1017/jns.2014.37. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 27. Allaway D, Gilham MS, Colyer A, et al. Metabolic profiling reveals effects of age, sexual development and neutering in plasma of young male cats. PLoS One 2016; 11. DOI: 10.1371/journal.pone.0168144. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 28. de Godoy MR, Shoveller AK. Overweight adult cats have significantly lower voluntary physical activity than adult lean cats. J Feline Med Surg 2017; 19: 1267–1273. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 29. Teixeira FA, Queiroz MR, Oba PM, et al. Brazilian owners perception of the body condition score of dogs and cats. BMC Vet Res 2020; 16: 463. DOI: 10.1186/s12917-020-02679-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 30. Teng KT, McGreevy PD, Toribio JLML, et al. Positive attitudes towards feline obesity are strongly associated with ownership of obese cats. PLoS One 2020; 15. DOI: 10.1371/journal.pone.0234190. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 31. Machado DS, Gonçalves LDS, Vicentini RR, et al. Beloved whiskers: management type, care practices and connections to welfare in domestic cats. Animals (Basel) 2020; 10. DOI: 10.3390/ani10122308. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 32. Chiang CF, Villaverde C, Chang WC, et al. Prevalence, risk factors, and disease associations of overweight and obesity in cats that visited the Veterinary Medical Teaching Hospital at the University of California, Davis from January 2006 to December 2015. Top Companion Anim Med 2022; 47. DOI: 10.1016/j.tcam.2021.100620. [DOI] [PubMed] [Google Scholar]
· 33. Hoelmkjaer KM, Bjornvad CR. Management of obesity in cats. Vet Med (Auckl) 2014; 5: 97–107. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 34. Teng KT, McGreevy PD, Toribio JALML, et al. Associations of body condition score with health conditions related to overweight and obesity in cats. J Small Anim Pract 2018; 59: 603–615. [DOI] [PubMed] [Google Scholar]
· 35. O’Neill DG, Gunn-Moore D, Sorrell S, et al. Commonly diagnosed disorders in domestic cats in the UK and their associations with sex and age. J Feline Med Surg 2023; 25. DOI: 10.1177/1098612X231155016. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 36. Mizorogi T, Kobayashi M, Ohara K, et al. Effects of age on inflammatory profiles and nutrition/energy metabolism in domestic cats. Vet Med (Auckl) 2020; 11: 131–137. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 37. Backus RC, Cave NJ, Keisler DH. Gonadectomy and high dietary fat but not high dietary carbohydrate induce gains in body weight and fat of domestic cats. Br J Nutr 2007; 98: 641–650. [DOI] [PubMed] [Google Scholar]
· 38. Teng KT, McGreevy PD, Toribio JLML, et al. Risk factors for underweight and overweight in cats in metropolitan Sydney, Australia. Prev Vet Med 2017; 144: 102–111. [DOI] [PubMed] [Google Scholar]
· 39. Godfrey H, Morrow S, Abood SK, et al. Identifying the target population and preventive strategies to combat feline obesity. J Feline Med Surg 2024; 26. DOI: 10.1177/1098612X241228042. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 40. Verbrugghe A, Hesta M. Cats and carbohydrates: the carnivore fantasy? Vet Sci 2017; 4: 55. DOI: 10.3390/vetsci4040055. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 41. Salaun F, Blanchard G, Le Paih L, et al. Impact of macronutrient composition and palatability in wet diets on food selection in cats. J Anim Physiol Anim Nutr (Berl) 2017; 101: 320–328. [DOI] [PubMed] [Google Scholar]
· 42. Plantinga EA, Bosch G, Hendriks WH. Estimation of the dietary nutrient profile of free-roaming feral cats: possible implications for nutrition of domestic cats. Br J Nutr 2011; 106: S35–48. [DOI] [PubMed] [Google Scholar]
· 43. Hewson-Hughes AK, Hewson-Hughes VL, Miller AT, et al. Geometric analysis of macronutrient selection in the adult domestic cat, Felis catus. J Exp Biol 2011; 214: 1039–1051. [DOI] [PubMed] [Google Scholar]
· 44. Hoenig M, Thomaseth K, Waldron M, et al. Insulin sensitivity, fat distribution, and adipocytokine response to different diets in lean and obese cats before and after weight loss. Am J Physiol Regul Integr Comp Physiol 2007; 292: R227–R234. [DOI] [PubMed] [Google Scholar]
· 45. Verbrugghe A, Hesta M, Van Weyenberg S, et al. The glucose and insulin response to isoenergetic reduction of dietary energy sources in a true carnivore: the domestic cat (Felis catus). Br J Nutr 2010; 104: 214–221. [DOI] [PubMed] [Google Scholar]
· 46. Nguyen PG, Dumon HJ, Siliart BS, et al. Effects of dietary fat and energy on body weight and composition after gonadectomy in cats. Am J Vet Res 2004; 65: 1708–1713. [DOI] [PubMed] [Google Scholar]
· 47. Mo R, Zhang M, Wang H, et al. Short-term changes in dietary fat levels and starch sources affect weight management, glucose and lipid metabolism, and gut microbiota in adult cats. J Anim Sci 2023; 101. DOI: 10.1093/jas/skad276. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 48. Coradini M, Rand JS, Morton JM, et al. Effects of two commercially available feline diets on glucose and insulin concentrations, insulin sensitivity and energetic efficiency of weight gain. Br J Nutr 2011; 106 Suppl 1: S64–S77. [DOI] [PubMed] [Google Scholar]
· 49. Puhl RM, Heuer CA. The stigma of obesity: a review and update. Obesity (Silver Spring) 2009; 17: 941–964. [DOI] [PubMed] [Google Scholar]
· 50. Frankel LA, O’Connor TM, Chen TA, et al. Parents’ perceptions of preschool children’s ability to regulate eating. Feeding style differences. Appetite 2014; 76: 166–174. [DOI] [PubMed] [Google Scholar]
· 51. Hughes SO, Shewchuk RM, Baskin ML, et al. Indulgent feeding style and children’s weight status in preschool. J Dev Behav Pediatr 2008; 29: 403–410. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 52. Rowe EC, Browne WJ, Casey RA, et al. Early-life risk factors identified for owner-reported feline overweight and obesity at around two years of age. Prev Vet Med 2017; 143: 39–48. [DOI] [PubMed] [Google Scholar]
· 53. Vague J. The degree of masculine differentiation of obesities: a factor determining predisposition to diabetes, atherosclerosis, gout, and uric calculous disease. Am J Clin Nutr 1956; 4: 20–34. [DOI] [PubMed] [Google Scholar]
· 54. Blüher M. Metabolically healthy obesity. Endocr Rev 2020; 41. DOI: 10.1210/endrev/bnaa004. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 55. Rey-López JP, de Rezende LF, Pastor-Valero M, et al. The prevalence of metabolically healthy obesity: a systematic review and critical evaluation of the definitions used. Obes Rev 2014; 15: 781–790. [DOI] [PubMed] [Google Scholar]
· 56. Smith GI, Mittendorfer B, Klein S. Metabolically healthy obesity: facts and fantasies. J Clin Invest 2019; 129: 3978–3989. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 57. Zoran DL. Obesity in dogs and cats: a metabolic and endocrine disorder. Vet Clin North Am Small Anim Pract 2010; 40: 221–239. [DOI] [PubMed] [Google Scholar]
· 58. Öhlund M, Egenvall A, Fall T, et al. Environmental risk factors for diabetes mellitus in cats. J Vet Intern Med 2017; 31: 29–35. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 59. Radakovich LB, Truelove MP, Pannone SC, et al. Clinically healthy overweight and obese dogs differ from lean controls in select CBC and serum biochemistry values. Vet Clin Pathol 2017; 46: 221–226. [DOI] [PubMed] [Google Scholar]
· 60. Busatto S, Walker SA, Grayson W, et al. Lipoprotein-based drug delivery. Adv Drug Deliv Rev 2020; 159: 377–390. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 61. Stadler JT, Marsche G. Obesity-related changes in high-density lipoprotein metabolism and function. Int J Mol Sci 2020; 21. DOI: 10.3390/ijms21238985. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 62. Ahmed B, Sultana R, Greene MW. Adipose tissue and insulin resistance in obese. Biomed Pharmacother 2021; 137. DOI: 10.1016/j.biopha.2021.111315. [DOI] [PubMed] [Google Scholar]
· 63. Gomes VDR, Ariza PC, Borges NC, et al. Risk factors associated with feline urolithiasis. Vet Res Commun 2018; 42: 87–94. [DOI] [PubMed] [Google Scholar]
· 64. Burggraaf ND, Westgeest D, Corbee RJ. Analysis of 7866 feline and canine uroliths submitted between 2014 and 2020 in the Netherlands. Res Vet Sci 2021; 137: 86–93. [DOI] [PubMed] [Google Scholar]
· 65. Piyarungsri K, Tangtrongsup S, Thitaram N, et al. Prevalence and risk factors of feline lower urinary tract disease in Chiang Mai, Thailand. Sci Rep 2020; 10: 196. DOI: 10.1038/s41598-019-56968-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 66. Pérez-López L, Boronat M, Melián C, et al. Kidney function and glucose metabolism in overweight and obese cats. Vet Q 2020; 40: 132–139. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 67. Markus MRP, Ittermann T, Baumeister SE, et al. Prediabetes is associated with microalbuminuria, reduced kidney function and chronic kidney disease in the general population: the KORA (Cooperative Health Research in the Augsburg Region) F4-Study. Nutr Metab Cardiovasc Dis 2018; 28: 234–242. [DOI] [PubMed] [Google Scholar]
· 68. Scarlett JM, Donoghue S. Associations between body condition and disease in cats. J Am Vet Med Assoc 1998; 212: 1725–1731. [PubMed] [Google Scholar]
· 69. Lund EM, Armstrong PJ, Kirk CK, et al. Prevalence and risk factors for obesity in adult cats from private US veterinary practices. Intern J Appl Res Vet Med 2005; 3: 88–96. [Google Scholar]
· 70. Zhang A, Silverberg JI. Association of atopic dermatitis with being overweight and obese: a systematic review and metaanalysis. J Am Acad Dermatol 2015; 72: 606–616.e4. [DOI] [PubMed] [Google Scholar]
· 71. Bennett D, Zainal Ariffin SM, Johnston P. Osteoarthritis in the cat: 1. how common is it and how easy to recognise? J Feline Med Surg 2012; 14: 65–75. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 72. Bonecka J, Skibniewski M, Zep P, et al. Knee joint osteoarthritis in overweight cats: the clinical and radiographic findings. Animals (Basel) 2023; 13. DOI: 10.3390/ani13152427. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 73. Lascelles BD, Henry JB, 3rd, Brown J, et al. Cross-sectional study of the prevalence of radiographic degenerative joint disease in domesticated cats. Vet Surg 2010; 39: 535–544. [DOI] [PubMed] [Google Scholar]
· 74. Slingerland LI, Hazewinkel HA, Meij BP, et al. Cross-sectional study of the prevalence and clinical features of osteoarthritis in 100 cats. Vet J 2011; 187: 304–309. [DOI] [PubMed] [Google Scholar]
· 75. Vina ER, Kwoh CK. Epidemiology of osteoarthritis: literature update. Curr Opin Rheumatol 2018; 30: 160–167. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 76. Frye CW, Shmalberg JW, Wakshlag JJ. Obesity, exercise and orthopedic disease. Vet Clin North Am Small Anim Pract 2016; 46: 831–841. [DOI] [PubMed] [Google Scholar]
· 77. Maniaki E, Murrell J, Langley-Hobbs SJ, et al. Associations between early neutering, obesity, outdoor access, trauma and feline degenerative joint disease. J Feline Med Surg 2021; 23: 965–975. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 78. Chandler ML. Impact of obesity on cardiopulmonary disease. Vet Clin North Am Small Anim Pract 2016; 46: 817–830. [DOI] [PubMed] [Google Scholar]
· 79. Atkins CE, Gallo AM, Kurzman ID, et al. Risk factors, clinical signs, and survival in cats with a clinical diagnosis of idiopathic hypertrophic cardiomyopathy: 74 cases (1985–1989). J Am Vet Med Assoc 1992; 201: 613–618. [PubMed] [Google Scholar]
· 80. Jordan E, Kley S, Le NA, et al. Dyslipidemia in obese cats. Domest Anim Endocrinol 2008; 35: 290–299. [DOI] [PubMed] [Google Scholar]
· 81. Finn E, Freeman LM, Rush JE, et al. The relationship between body weight, body condition, and survival in cats with heart failure. J Vet Intern Med 2010; 24: 1369–1374. [DOI] [PubMed] [Google Scholar]
· 82. García-Guasch L, Caro-Vadillo A, Manubens-Grau J, et al. Pulmonary function in obese vs non-obese cats. J Feline Med Surg 2015; 17: 494–499. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 83. Caro-Vadillo A, Montoya-Alonso JA, García-Guasch L. Impact of obesity on lung function in cats with bronchoconstriction. Vet Sci 2022; 9. DOI: 10.3390/vetsci9060278. [DOI] [PMC free article] [PubMed] [Google Scholar]
· 84. Arismendi E, Bantulà M, Picado C. Obese asthma syndrome: much work to do. Arch Bronconeumol 2023; 59: 473–475. [DOI] [PubMed] [Google Scholar]
· 85. Ishioka K, Omachi A, Sasaki N, et al. Feline adiponectin: molecular structures and plasma concentrations in obese cats. J Vet Med Sci 2009; 71: 189–194. [DOI] [PubMed] [Google Scholar]
· 86. Hoenig M, Pach N, Thomaseth K, et al. Cats differ from other species in their cytokine and antioxidant enzyme response when developing obesity. Obesity (Silver Spring) 2013; 21: E407–E414. [DOI] [PubMed] [Google Scholar]
· 87. Appleton DJ, Rand JS, Sunvold GD. Insulin sensitivity decreases with obesity, and lean cats with low insulin sensitivity are at greatest risk of glucose intolerance with weight gain. J Feline Med Surg 2001; 3: 211–228. [DOI] [PMC free article] [PubMed] [Google Scholar]
Articles from Journal of Feline Medicine and Surgery are provided here courtesy of SAGE Publications








